Ebola outbreaks are considered rare, but they do emerge every several years and can be quite lethal. Although the first confirmed Ebola epidemic was in 1976, we still lack licensed therapeutics to prevent and control Ebola’s spread. Vaccine development is in the works, but the lack of an approved treatment is a chilling reminder that we may not know enough about the virus. With the recent outbreaks in mind, we sought to summarize everything you should know about Ebola, its biology, and the current progress of vaccine development.
Edit (April 11, 2019): This post has been updated in light of recent Ebola outbreaks and developments.
What is Ebola?
Ebola is one of the world’s most virulent diseases. The Ebolavirus belongs to the order Mononegavirales and family Filoviridae, a group of enveloped, negative-strand RNA viruses. The single-stranded RNA (ssRNA) is composed of only seven genes which are all monocistronic (only codes for a single protein) with the exception of the glycoprotein. There are six known strains of Ebolavirus (listed below), four of which can cause Ebola viral disease (EBV) in humans. EBV is considered rare, but it is also highly fatal, killing 50% of infected patients on average.
Ebolavirus Strains
- Zaire ebolavirus (EBOV)
- Sudan ebolavirus (SUDV)
- Tai Forest ebolavirus, formerly Cote d’Ivoire ebolavirus (TAFV)
- Bundibugyo ebolavirus (BDBV)
- Reston ebolavirus (RESTV). (infects nonhuman primates)
- Bombali ebolavirus
Ebolavirus genes
- Nucleoprotein
- Glycoprotein
- Virion proteins (VP):
- VP24
- VP30
- VP35
- VP40
- RNA-dependent RNA polymerase
Although the natural reservoir for Ebolaviruses remains unconfirmed, the disease is transmitted through contact with the bodily fluids of infected animals and humans. Along with influenza-like symptoms, EBV also leads to internal and external bleeding, severe dehydration, and in some cases, multiorgan failure.
More about the symptoms and disease progression here.
How Ebola Infects: Entering and Breaking
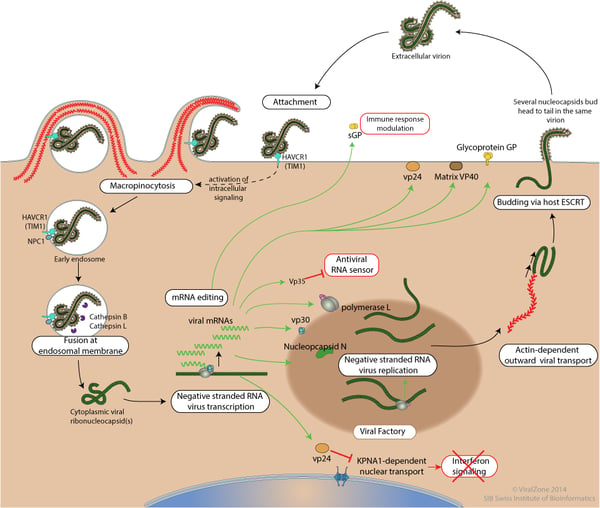
Like many viruses, Ebola’s ultimate goal is to create numerous copies of itself so that it may spread rapidly to other hosts. In order to accomplish this mission, the Ebola virus, which does not have its own replication machinery, makes use of the host (the infected subject) and hijacks the host’s cells transcriptional enzymes.
Entering
The first step is to enter the cell. Ebolavirus does this by exploiting a cellular process called macropinocytosis, which is usually reserved for nutrient uptake. After attachment to the cell’s receptors, the virus awaits to be “ingested.” In this process, an extension of the cell’s membrane wraps around the virus and fully surrounds it, forming a small compartment which is then transported into the cytosol (and thus becoming an endosome).
Once inside the cell, the virus breaks free of the endosome and begins its replication mission by using the cell’s transcriptional enzymes. First, the viral ssRNA is transcribed into its seven proteins as mentioned previously. Among these proteins is the nucleoprotein which is essential to forming the nucleocapsid which envelops the viral RNA. After viral protein levels increase and enough nucleoprotein and glycoproteins are present, RNA-dependent RNA polymerase (which was just transcribed) starts to replicate the viral RNA.
Breaking
Once enough copies are made, the viral RNAs and membrane forming proteins gather at the host cell’s plasma membrane to assemble and exit the cell through budding. In budding, the virus steals the host cell’s plasma membrane, which encloses the virion. For this step, the virus continues to hijack the host cell’s machinery by using components of the cellular ESCRT (endosomal sorting complex required for transport). Finally, the replicated viruses exit the cell, destroying it along the way. With Ebola, the sheer quantity of cells bursting is so immense that it prompts an inflammatory response which causes flu-like symptoms.
Why is Ebola so deadly?
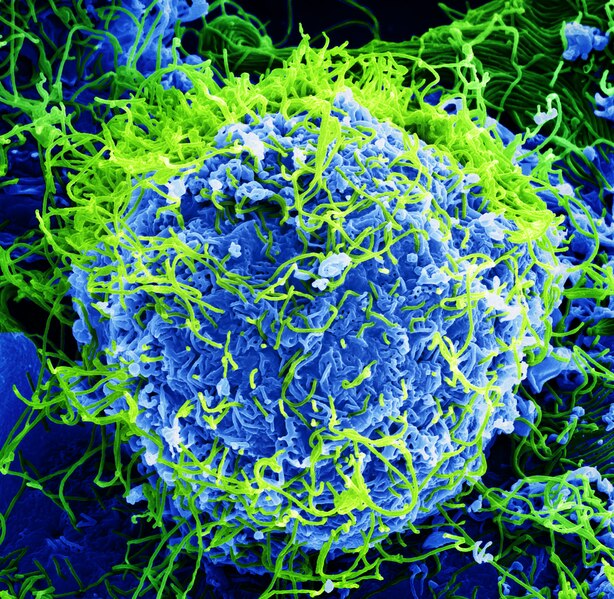
Ebola is a swift and effective killer, having mastered the art of evasion. Upon entering the host body, the Ebola virus targets dendritic cells - antigen-presenting cells that serve as the body’s first line of defense against foreign invasion. Dendritic process and present antigen materials to the body’s white blood cells. The white blood cells (T cells to be exact) are then able to initiate an immune response involving antibody activation.
However, with defective dendritic cells, there is no way to trigger an immune response. Like many other viruses, Ebola also interferes with the cell’s production of interferon, a signaling protein that alerts neighboring cells to amplify their anti-viral defenses. Of Ebola's seven monocistronic genes, one codes for viral protein 24 (VP24), responsible for blocking interferon signaling. By compromising the host’s immune system, the Ebola virus can replicate and spread quickly without much resistance.
For infected patients, the most threatening aspect of Ebola is death-inducing hemorrhaging. Ebola infection can cause blood clotting, which clogs and ruptures blood vessels. Glycoproteins attach to the inside of blood vessels increasing permeability, leading to vessel breakage.
Are there Ebola vaccines?
While development is ongoing, there is no licensed or clinically approved vaccine. Many experimental vaccines are in clinical trials, but studies have previously halted due to insufficient participants or other trial delays.
Currently in use: mAb114
The mAb114 treatment is a monoclonal antibody which was isolated from a human survivor from the 1995 Ebola outbreak in the Democratic Republic of Congo (DRC). It is currently being offered to patients in the DRC outbreak as part of a Phase 2/3 trial, under compassionate care. More on mAb114.
.jpg)



.png)