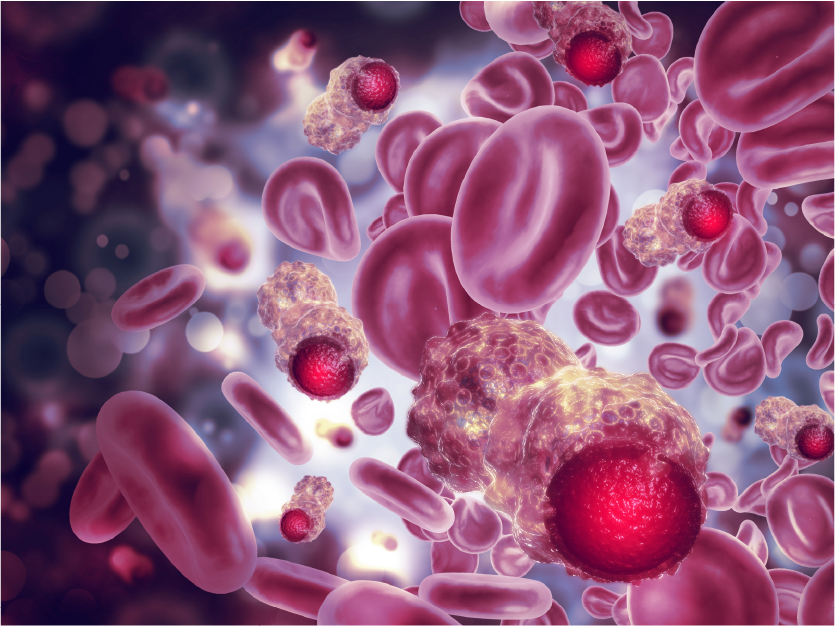
 As science advances, one of the recent trends that continues to pay dividends is immunotherapy to fight cancers. In many cases, the strategy is to mobilize the immune system to attack tumor cells based on cancer-specific antigens expressed either by the tumor itself or within the tumor microenvironment, either by stimulating normal immune cell function to their new tumor target or by removing the suppression of the immune system that is characteristic of many cancers. The trick is to find a way to attack only the tumor and not normal tissues, and certainly not to somehow trigger autoimmunity.
As science advances, one of the recent trends that continues to pay dividends is immunotherapy to fight cancers. In many cases, the strategy is to mobilize the immune system to attack tumor cells based on cancer-specific antigens expressed either by the tumor itself or within the tumor microenvironment, either by stimulating normal immune cell function to their new tumor target or by removing the suppression of the immune system that is characteristic of many cancers. The trick is to find a way to attack only the tumor and not normal tissues, and certainly not to somehow trigger autoimmunity.
The Role of IL-15 in Immunity
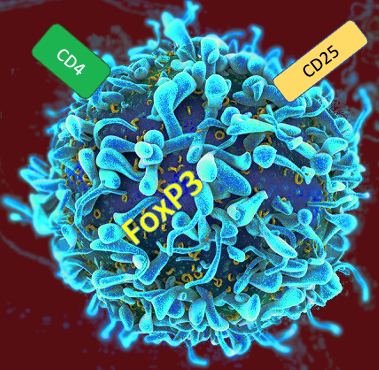
We did something similar with CCR8 in anti-tumor targeted therapy, and now we have a new pet molecule in interleukin 15, or IL-15 for short. IL-15 is structurally similar to IL-2, which activates T cells, and is itself a pro-inflammatory cytokine. Like other interleukins, IL-15 plays a significant role in mediating immune function either on its own or in combination with other cytokines. IL-15 can activate CD8 T cells and natural killer (NK) cells, but unlike IL-2, does not cause activation-induced cell death or activate regulatory T (Treg) cells. There are multiple isoforms of IL-15 and its receptor, and each isoform can modulate different functions ranging from signal transduction to cytokine secretion.
IL-15 as a Therapeutic Target
 The challenge with using IL-15 as a therapy stems from its short half-life and tight control over its expression, but recent efforts have begun to overcome these obstacles as new drugs are being designed to take advantage of IL-15's abilities. While IL-2 was initially used as an immunotherapy, IL-15 confers certain advantages, including a lack of major cytotoxicity and avoiding the stimulation of Tregs. The lower cytotoxicity makes IL-15 a safer alternative to IL-2, while its ability to mobilize antitumor cells is maintained.
The challenge with using IL-15 as a therapy stems from its short half-life and tight control over its expression, but recent efforts have begun to overcome these obstacles as new drugs are being designed to take advantage of IL-15's abilities. While IL-2 was initially used as an immunotherapy, IL-15 confers certain advantages, including a lack of major cytotoxicity and avoiding the stimulation of Tregs. The lower cytotoxicity makes IL-15 a safer alternative to IL-2, while its ability to mobilize antitumor cells is maintained.
IL-15 has been amazingly effective in many human trials, following from its success in reducing tumor burden while improving survival outcomes. The indicators upon IL-15 treatment are logical, with increases in the circulating NK cell and both CD4 and CD8 T cell populations, plus the upregulation of other pro-inflammatory cytokines, and in many cases, even without major tumor reduction, the disease was at least stabilized. IL-15 seemed to be much more effective in combination therapy, as is the norm in recent times in treating advanced cancers that may be resistant to singular therapies. This can be done in concert with other immune agonists, checkpoint inhibitors, or anticancer monoclonal antibody therapies. Though, as with all areas of biology, more research needs to be performed, IL-15 therapies are a popular research focus and the safety and effectiveness evidenced in the scientific record and in clinical trials cannot be ignored.
A Promising New IL-15 Immunotherapy for Bladder Cancer
As a locally secreted molecule, IL-15 lends itself to being manipulated to more selectively target tumors. My college buddy from UC Berkeley, Philip Liu, Ph.D., now works with ImmunityBio, a company whose mission is developing therapies that kill the disease and not the immune system. One of their current projects that is about to enter clinical trials is an IL-15 superagonist therapy against bladder cancer, which Phil graciously discusses with us on this episode of BioChat. We also lament the disparities in research funding, as Phil used to be a university professor, while talking about our shared love of science and the immune system. You can learn how to subscribe to our podcast at our BioChat page.
References