 The dream of biomedical researchers is to fine-tune their therapeutics to precisely target the specific illness or pathogen affecting their patient. Ever since Nobel laureate and oft-quoted father of immunology, Paul Ehrlich, coined the term “magic bullet,” medical science has marched towards more personalized drugs that target key molecules that cause diseases including cancer. 1 We find ourselves now, over a century later, in an exciting era of discovery that has produced many antibody drug conjugates (ADC) designed to precisely target the diseased cells and not healthy cells. ADC uses this strategy to take advantage of the specificity of antibodies while delivering a covalently linked cytotoxic payload directly to diseased tissues to reduce the multitudes of side effects and toxicity. 2, 3 As basic research identifies more targets and antibody engineering procedures improve, the range of antitumor and anti-disease weapons may seem limitless.
The dream of biomedical researchers is to fine-tune their therapeutics to precisely target the specific illness or pathogen affecting their patient. Ever since Nobel laureate and oft-quoted father of immunology, Paul Ehrlich, coined the term “magic bullet,” medical science has marched towards more personalized drugs that target key molecules that cause diseases including cancer. 1 We find ourselves now, over a century later, in an exciting era of discovery that has produced many antibody drug conjugates (ADC) designed to precisely target the diseased cells and not healthy cells. ADC uses this strategy to take advantage of the specificity of antibodies while delivering a covalently linked cytotoxic payload directly to diseased tissues to reduce the multitudes of side effects and toxicity. 2, 3 As basic research identifies more targets and antibody engineering procedures improve, the range of antitumor and anti-disease weapons may seem limitless.
Commercially Available Antibody-Drug Conjugates
There have been huge advances in the understanding of ADC development and in 2021 alone, 14 ADC products have been approved, including 10 by the US Food and Drug Administration. 2-4 As of August of 2023, there are now 11 FDA-approved ADCs with targets such as CD19, CD22, CD30, CD33, and CD79b for the treatment of hematological malignancies such as leukemia, while in solid tumors, particularly breast cancer, the target is usually HER2. 5
 Mylotarg, from Pfizer, is the first approved ADC on the market. This ADC is a humanized anti-CD33 antibody linked to the DNA damaging molecule calicheamicin and is designed to treat acute myeloid leukemia. This pioneering therapeutic was designed in the 1990s, with FDA approval coming in 2000 to kickstart the next two decades of ADC development. Mylotarg has been the subject of some controversy and scrutiny over the intervening years due to serious side effects that could lead to fatality, but continuous improvements to the drug design have kept it in global use.
Mylotarg, from Pfizer, is the first approved ADC on the market. This ADC is a humanized anti-CD33 antibody linked to the DNA damaging molecule calicheamicin and is designed to treat acute myeloid leukemia. This pioneering therapeutic was designed in the 1990s, with FDA approval coming in 2000 to kickstart the next two decades of ADC development. Mylotarg has been the subject of some controversy and scrutiny over the intervening years due to serious side effects that could lead to fatality, but continuous improvements to the drug design have kept it in global use.
A particularly successful ADC is the AstraZeneca drug marketed as Enhertu, which consists of the anti-HER2 antibody trastuzumab connected to a topoisomerase I inhibitor as a method of fighting breast cancer. Designed for the treatment of HER2-positive cancers that were metastatic or unable to be surgically removed, Enhertu was approved by the FDA in 2019. Since then, Enhertu has also been approved for HER2-positive gastric and esophageal cancers in patients who had received previous HER2-based treatments.
One of the most commercially successful ADCs on the market is Kadcyla, or trastuzumab emtansine, from Genentech. In 2021, the global ADC market was over $5.2 billion, with Kadcyla sales making up $2.17 billion of that total. Another HER2-based treatment against breast cancer, Kadcyla employs a potent microtubule inhibitor to disrupt mitosis.
Although ADCs continue to display various side effects in patients receiving treatment, the efficacy in reducing disease recurrence and improving patient survival rates is evident and make this class of therapeutic attractive for future study. Per the Kadcyla release, ADCs including Kadcyla will still generate billions in revenue, but growth might be limited because of high pricing that has made it difficult to adopt the drug in certain areas of the world, and the rise of biosimilars on the market to provide a “generic” alternative to the name-brand drug.
A Shift in Focus for Antibody-Drug Conjugates
To stay ahead of the biosimilar trend, companies need to continue to innovate new targets in an effort to keep expanding their existing portfolio and maximize their market share. For instance, Daiichi Sankyo, the company that helped AstraZeneca develop Enhertu, is looking into novel targets that aren’t HER2, such as TROP2 with their datopotamab deruxtecan, branded Dato-DXd, as well as a patritumab deruxtecan to target HER3. Daiichi is expecting to corner the ADC market with sales exceeding $10 billion by 2029.
 Commonly in today’s pharmaceutical landscape, companies are collaborating, merging, or being absorbed by larger companies in the pursuit of resource sharing and profit. In October 2023, Glaxo Smith Kline (GSK) formed an exclusive license agreement with Chinese company Hansoh Pharma to market HS-20089, a B7-H4 targeted ADC undergoing Phase I trials in China. GSK plans to also perform Phase I trials outside of China in 2024. This drug is showing promising early results in combatting ovarian and endometrial cancer by targeting the ovarian marker B7-H4 with a topoisomerase inhibitor payload. GSK paid out $85 million up front, and Hansoh stands to earn over a billion dollars in success-based milestones.
Commonly in today’s pharmaceutical landscape, companies are collaborating, merging, or being absorbed by larger companies in the pursuit of resource sharing and profit. In October 2023, Glaxo Smith Kline (GSK) formed an exclusive license agreement with Chinese company Hansoh Pharma to market HS-20089, a B7-H4 targeted ADC undergoing Phase I trials in China. GSK plans to also perform Phase I trials outside of China in 2024. This drug is showing promising early results in combatting ovarian and endometrial cancer by targeting the ovarian marker B7-H4 with a topoisomerase inhibitor payload. GSK paid out $85 million up front, and Hansoh stands to earn over a billion dollars in success-based milestones.
In an example of a big company flexing its financial muscle, Eli Lilly is snatching up ADC startup companies, first with Emergence Therapeutics and then Mablink Bioscience as of October 2023. The primary goal of this acquisition seems to be the Mablink linker technology, which hopes to reduce toxicity and improve drug delivery to cancer cells. Similarly, BioNTech is also entering a licensing agreement with MediLink Therapeutics for their HER3-based non-small cell lung cancer and breast cancer ADC, with particular interest in their linker technology that is activated by enzymes within the tumor microenvironment.
Challenges in Developing Effective Antibody-Drug Conjugates
The ideal ADC relies on an effective, specific antibody that preferentially targets the biomarker on diseased cells relative to healthy cells, minimizing any off-target effects that could be detrimental to the patient. Modern strategies take advantage of the consistency and superior specificity of monoclonal antibodies, where researchers can reduce their concerns about non-specific binding or off-target effects and the pool of antibodies used is identical. For use in human patients, the antibody itself can be humanized to improve the antibody’s effector functions and stability in the host without triggering an adverse immune response. There has been a shift towards using rabbit as the antibody-generating host, due in part to the superior affinity, specificity, and the more diverse range of antigenic recognition of rabbit antibodies compared to mouse.
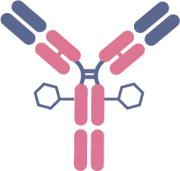 A related challenge is in the effective delivery of the payload to the disease site, due in part to the large size of the antibody itself. One potential strategy is to reduce the size of the antibody. The strategy could employ camelid-derived nanobodies, which retain the antigen-recognition function of an antibody but are a fraction the size of a conventional antibody. An additional rate-limiting step in ADC development is the design of the chemical linker, where the premature release of the cytotoxic drug could lead to severe side effects including hematotoxicity. 3 The importance of an effective linker is evident in the recent industry acquisitions we discussed earlier.
A related challenge is in the effective delivery of the payload to the disease site, due in part to the large size of the antibody itself. One potential strategy is to reduce the size of the antibody. The strategy could employ camelid-derived nanobodies, which retain the antigen-recognition function of an antibody but are a fraction the size of a conventional antibody. An additional rate-limiting step in ADC development is the design of the chemical linker, where the premature release of the cytotoxic drug could lead to severe side effects including hematotoxicity. 3 The importance of an effective linker is evident in the recent industry acquisitions we discussed earlier.
The Future of Antibody-Drug Conjugates
The lessons learned from the early Mylotarg trials may explain why it was another decade before a second ADC was approved, but the field has accelerated since. Currently, there are over 100 ADC therapeutics in clinical trials in addition to the handful that have been approved. Most of these are from the usual suspects in large pharmaceutical companies like Bristol-Myers Squibb and Roche, but there are some academic institutions like the National Cancer Center and the Mayo Clinic chipping in as well. Like Enhertu, many other ADC strategies center around HER2. One example is Aidixi from RemeGen, which is a humanized anti-HER2 antibody connected to the antimitotic agent monomethyl auristatin E (MMAE) and approved in China for the treatment of advanced gastric cancer.
 Basic research is still necessary to focus development efforts into novel targets. To alleviate the market saturation surrounding HER2 and other common targets such as EGFR, many of the current ADC projects in clinical trials are focusing on markers such as tissue factor, Trop-2, CEACAM5, and more. 3 It is remarkable that there was a significant increase in the number of journal articles with an even larger increase in patents for ADCs. Improving the diversity of antitumor antibodies while reducing toxicity to patients is critical to the success of future ADC treatments. 3, 4
Basic research is still necessary to focus development efforts into novel targets. To alleviate the market saturation surrounding HER2 and other common targets such as EGFR, many of the current ADC projects in clinical trials are focusing on markers such as tissue factor, Trop-2, CEACAM5, and more. 3 It is remarkable that there was a significant increase in the number of journal articles with an even larger increase in patents for ADCs. Improving the diversity of antitumor antibodies while reducing toxicity to patients is critical to the success of future ADC treatments. 3, 4
From a business growth point of view, the global ADC market was estimated to be worth $8.6 billion in 2022, with projections at $23.9 billion by 2032. The promise of these drugs cannot be ignored, and with more effective delivery, linkage, and reduction in toxicity, there is plenty of potential to improve the well-being of not only cancer patients, but perhaps in many other diseases as well.
How ABclonal Can Help
![]() Take advantage of ABclonal’s SMab™ platform to generate your desired recombinant monoclonal antibody weapon, with complimentary antigen design to help you validate the feasibility of your target. ABclonal can help you engineer your antibody to the necessary specifications, as well as assist in pharmacokinetic analysis for your assembled ADC. If you are concerned about the size of the antibody that could affect delivery and potency of your ADC, please also consider trying our camelid nanobody service. You can visit any of those links to inquire about a quote. For more information, please don’t hesitate to contact us at service@abclonal.com!
Take advantage of ABclonal’s SMab™ platform to generate your desired recombinant monoclonal antibody weapon, with complimentary antigen design to help you validate the feasibility of your target. ABclonal can help you engineer your antibody to the necessary specifications, as well as assist in pharmacokinetic analysis for your assembled ADC. If you are concerned about the size of the antibody that could affect delivery and potency of your ADC, please also consider trying our camelid nanobody service. You can visit any of those links to inquire about a quote. For more information, please don’t hesitate to contact us at service@abclonal.com!
References
- Strebhardt K & Ullrich A (2008) “Paul Ehrlich’s magic bullet concept: 100 years of progress.” Nature Reviews Cancer 8:473-480.
- Pettinato MC (2021) “Introduction to Antibody-Drug Conjugates.” Antibodies (Basel) 10(4):42 (Epub).
- Fu et al. (2022) “Antibody drug conjugate: the ‘biological missile’ for targeted cancer therapy.” Signal Transduction and Targeted Therapy 7:93 (Epub).
- Shastry et al. (2023) “Rise of Antibody-Drug Conjugates: The Present and Future.” American Society of Clinical Oncology Educational Book 43 (Epub).
- Gogia et al. (2023) “Antibody-Drug Conjugates: A Review of Approved Drugs and Their Clinical Level of Evidence.” Cancers (Basel) 15(15):3886 (Epub).

.png)