December is a month of holidays and celebration, but it is also a time to raise awareness for a global epidemic that has lasted over four decades. During World HIV/AIDS Awareness Month, health organizations, including the United States Department of Veteran Affairs, serve to remind everyone about the importance of getting tested, to remember those who succumbed to the disease, and to improve access to advanced therapies.
December is a month of holidays and celebration, but it is also a time to raise awareness for a global epidemic that has lasted over four decades. During World HIV/AIDS Awareness Month, health organizations, including the United States Department of Veteran Affairs, serve to remind everyone about the importance of getting tested, to remember those who succumbed to the disease, and to improve access to advanced therapies.
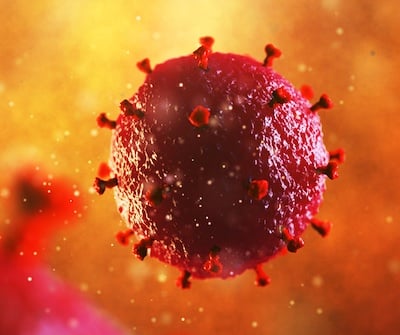
Since its first identification and description in 1981, medical advances have offered effective therapies to keep the virus at bay, and in some cases even completely cure a patient of the human immunodeficiency virus, or HIV, and to prevent it from becoming the acquired immunodeficiency syndrome, or AIDS, which is often catastrophic to the patient. Unfortunately, as of 2021 per the World Health Organization (WHO), there are still over 38 million people living with HIV, with approximately 1.5 million new infections and 650,000 HIV-related deaths. Much of this has to do with lack of education or proper infrastructure and often obstacles to accessibility for treatment and prevention. I hope to explore HIV with you during this month of awareness so we can do our part to mitigate this persistent epidemic.
Government Policies to Fight HIV
I was intrigued to find that there is a dedicated website to the American government strategy to combat HIV. Harold Phillips is the Director of the White House Office of National AIDS Policy (ONAP) and has set up a top five priorities list to tackle this epidemic:
- Achieving health equity with a focus on populations and jurisdictions with the greatest need.
- Increasing the uptake of PrEP among those who could benefit from this prevention method.
- Accelerating public/private partnerships to help reach communities most impacted by HIV.
- Increasing access to substance use disorder treatment and mental health services.
- Modernizing and repealing outdated HIV criminalization laws.
This priority list aligns with the National HIV/AIDS Strategy set up by the President with a goal of ending the HIV epidemic in the United States by the year 2030. The immediate goal is to prevent new HIV infections, to ensure everyone can get tested, knows their status with respect to the virus, receives treatment needed to maintain quality of life, and hopefully through education, reduce the prejudice against people living with the disease. This strategy acts in concert with academic institutions and biotech companies that develop the novel therapeutics to ensure that the patients in need will get the medicine they require.
Preventing HIV
 Although it is good to know there is a huge global awareness of the epidemic, individuals can also protect themselves while the health policies are being enacted. There are of course common sense practices to prevent transmittable diseases, especially since HIV is normally transmitted through sexual contact or contaminated drugs or fluids. Given the availability of testing and your own due diligence, HIV is extremely preventable.
Although it is good to know there is a huge global awareness of the epidemic, individuals can also protect themselves while the health policies are being enacted. There are of course common sense practices to prevent transmittable diseases, especially since HIV is normally transmitted through sexual contact or contaminated drugs or fluids. Given the availability of testing and your own due diligence, HIV is extremely preventable.
There are also first-line antiretroviral treatments to prevent transmission of HIV. You’ve probably seen those commercials for pre-exposure prophylaxis (PrEP) and there is also post-exposure prophylaxis (PEP) for folks who are sexually active but might fear contracting HIV. PrEP is taken prior to HIV exposure, while PEP is taken as soon as possible after suspected HIV exposure. Another potential therapy, leronlimab, could also work as a pre-exposure preventative drug, and studies are underway to determine whether this drug could be continuously manufactured through gene therapy. While both PrEP and PEP are highly effective, neither will completely eliminate the risk of infection, so again, common sense needs to prevail.
Treatment of HIV
There are various treatment strategies for patients living with HIV that keep the virus under control. Beyond small molecule inhibitors against the HIV protease or other viral proteins, many targeted therapies are based on broadly neutralizing monoclonal antibodies (bNAb) that are directed to HIV glycans or the co-receptor CCR5 that allows the virus to enter cells. 1, 2 There is a need to calibrate the dosage to achieve the level of viral control needed to maintain the patient’s health. 1
 In addition to antibody blockades, strategies involving gene editing techniques like CRISPR can attempt to delete HIV-facilitating genes (including CCR5) from susceptible cells to prevent future viral propagation. 2-4 Reprogramming stem cells via gene editing could help repopulate the host immune system with cells that are resistant to HIV re-infection, if the technique can overcome any pre-existing immunity to the therapeutics. 3-5
In addition to antibody blockades, strategies involving gene editing techniques like CRISPR can attempt to delete HIV-facilitating genes (including CCR5) from susceptible cells to prevent future viral propagation. 2-4 Reprogramming stem cells via gene editing could help repopulate the host immune system with cells that are resistant to HIV re-infection, if the technique can overcome any pre-existing immunity to the therapeutics. 3-5
There is some evidence that extracellular vesicles (EVs) may be an effective therapeutic agent. By transporting HIV restriction factors to nearby cells, or by presenting viral antigens on their surface, EVs may be able to stimulate antiviral responses. However, EV transport of HIV and its molecules throughout the host could also reactivate HIV, so fine-tuning the pro-viral and anti-viral effects would be critical to the success of this treatment strategy. 6 Presenting antigen more efficiently, possibly through the host dendritic cells, could serve as a therapeutic vaccine against HIV infection as it could activate the host immune system naturally to target a stronger response against the virus. 7
A Cure for HIV?
Many people are leading normal, healthy lives while living with the virus (Magic Johnson comes to mind) but there have been sprinkles of success stories as new techniques and therapies are reported in which the person not only thrives but is essentially free of the HIV that once infected them. While many of these stories give us hope, the patients would need to be tracked long term to ensure that HIV is not just lying dormant to strike again.
Pharmaceutical specialty companies like ViiV Healthcare are working not only on better treatments, but eventually a cure for HIV. One of the challenges is that HIV tends to mask itself within the host cells and remains dormant in a “latent reservoir” where it can rest until antiretroviral treatments stop, at which point the HIV can re-emerge and propagate again. Through massive collaboration, the goal is to trick HIV into presenting viral proteins that can allow the virus to be tagged and subsequently recognized by the host immune system for destruction. 8
 At City of Hope Hospital in California, a 66-year-old man living with HIV since 1988 showed remission from the virus for over 17 months following a stem cell transplant to treat his acute leukemia. The transplant was received over three years ago, and the patient was able to stop his antiretroviral treatments without the virus making a comeback. In this case, the tissue donor had a rare CCR5 delta 32 mutation that is resistant to HIV infection, which most likely contributed to the remission.
At City of Hope Hospital in California, a 66-year-old man living with HIV since 1988 showed remission from the virus for over 17 months following a stem cell transplant to treat his acute leukemia. The transplant was received over three years ago, and the patient was able to stop his antiretroviral treatments without the virus making a comeback. In this case, the tissue donor had a rare CCR5 delta 32 mutation that is resistant to HIV infection, which most likely contributed to the remission.
Combining multiple approaches, a group from Israel recently reported that they were able to edit B cells in live mice to begin secreting sufficient bNAbs to target HIV in their animal model. 9 Such a technique has yet to be tested in humans, but the initial results are encouraging and suggest that it could be applied to fight other types of diseases, including autoimmunity and cancer.
Of course, the holy grail of health science against any disease is a vaccine to prevent infection or illness before the virus can get a foothold. Recently, a Phase 1 clinical trial was published in Science Magazine that showed a safe and effective response in human patients in developing bNAbs against HIV antigens, hopefully paving the road to an eventual broadly administered vaccine to quell the epidemic once and for all!
The Battle Rages On
With over 40 years of research and advancement, we are likely to see more of these success stories as scientists and medical professionals fine-tune and master their gene editing techniques. The obstacle is in the delivery method and in ensuring safety, but the promise is apparent. With government policies and continued individual vigilance, HIV may one day be eradicated just as we did with other major human diseases.
References
- Julg et al. (2022) “Safety and antiviral activity of triple combination broadly neutralizing monoclonal antibody therapy against HIV-1: a phase 1 clinical trial.” Nat Med 28(6):1288-1296.
- Mohamed et al. (2021) “Targeting CCR5 as a Component of an HIV-1 Therapeutic Strategy.” Front Immunol 12:816515 (Epub).
- Kanula UR and Wake AD (2022) “Promising Stem Cell therapy in the Management of HIV and AIDS: A Narrative Review.” Biologics 16:89-105.
- Zhang Z, Hou W, and Chen S (2022) “Updates on CRISPR-based gene editing in HIV-1/AIDS therapy.” Virol Sin 37(1):1-10.
- Charlesworth et al. (2022) “Immunological barriers to haematopoietic stem cell gene therapy.” Nat Rev Immunol 2022 Mar 17:1-15 (Epub).
- Navarrete-Muñoz et al. (2021) “Extracellular Vesicles as a New Promising Therapy in HIV Infection.” Front Immunol 12:811471 (Epub).
- Espinar-Buitrago M and Muñoz-Fernández MA (2021) “New Approaches to Dendritic Cell-Based Therapeutic Vaccines Against HIV-1 Infection.” Front Immunol 12:719664 (Epub).
- Nixon et al. (2020) “Systemic HIV and SIV latency reversal via non-canonical NF-kB signalling in vivo.” Nature 578:160-165.
- Nahmad et al. (2022) “In vivo engineered B cells secrete high titers of broadly neutralizing anti-HIV antibodies in mice.” Nature Biotechnology 40:1241-1249.