As a scientist (or at least, a guy who likes science and works for a bioscience-oriented company), I am invested in the power of scientific research in improving the quality of human life across all arenas. It is particularly gratifying when our customers, who are all primarily research scientists, derive direct benefit from ABclonal's products in their published research. In this case, our business development director had a customer recently defend her thesis based on a publication that used several ABclonal catalog antibodies. I enjoyed reading her group's article that may lead to more effective treatment strategies for diabetes patients going forward, so let's get to it.
ABclonal in Action: Diabetes, Insulin, and Resisting Graft Rejection
Remember once upon a time when I said my first actual laboratory research project involved myelin basic protein? Other than knowing that the mother of one of my high school friends had been diagnosed with it, this was the first real exposure I had with multiple sclerosis. I eventually learned more about the immune system and autoimmunity, and the thought of your own body attacking your literal nerve cells was scary and made me feel for the people who have to live with and manage this disease every day. March happens to be Multiple Sclerosis Awareness Month, which as the name suggests works to make sure the public knows about multiple sclerosis, develops empathy and understanding for afflicted individuals, and encourages participation in events and activities to spread awareness. In this blog, let's explore the disease, current treatment strategies and ongoing research, and ways that you can help both in and out of the lab.
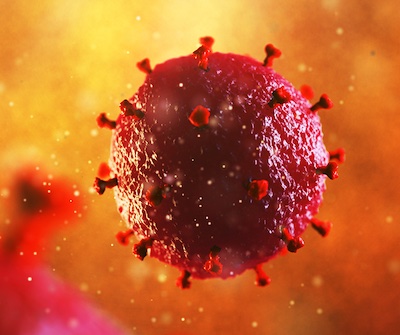
December is a month of holidays and celebration, but it is also a time to raise awareness for a global epidemic that has lasted over four decades. During World HIV/AIDS Awareness Month, health organizations, including the United States Department of Veteran Affairs, serve to remind everyone about the importance of getting tested, to remember those who succumbed to the disease, and to improve access to advanced therapies.
Since its first identification and description in 1981, medical advances have offered effective therapies to keep the virus at bay, and in some cases even completely cure a patient of the human immunodeficiency virus, or HIV, and to prevent it from becoming the acquired immunodeficiency syndrome, or AIDS, which is often catastrophic to the patient. Unfortunately, as of 2021 per the World Health Organization (WHO), there are still over 38 million people living with HIV, with approximately 1.5 million new infections and 650,000 HIV-related deaths. Much of this has to do with lack of education or proper infrastructure and often obstacles to accessibility for treatment and prevention. I hope to explore HIV with you during this month of awareness so we can do our part to mitigate this persistent epidemic.
With a background in both immunology and cancer biology, I’ve always had a fascination with the interplay between the body’s immune system and any tumors that might pop up. Originally, it made sense that the immune system would actively seek out and destroy cancerous cells, but the emerging consensus is that the interactions between cancers and host immunity is far more complex. In addition to growing new blood vessels and reprogramming metabolic processes, there appears to be some imbalance between avoiding immune cells while also promoting tumor-infiltrating inflammatory cells to promote its growth. 1 (Figure 1) Trying to dissect this apparent contradictory relationship between tumors and host immunity remains a hot topic.
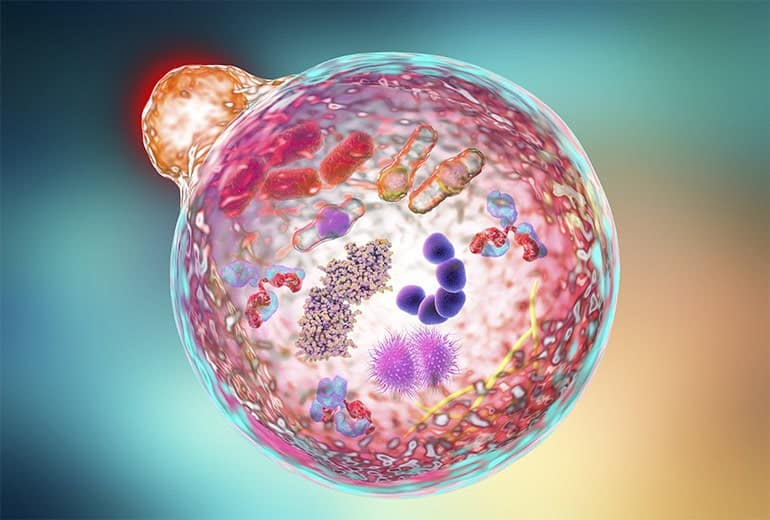
Autophagy can be understood as ‘self-eating’. In simple terms, it is a vitally important cleansing mechanism carried out by the cells in our body. It brings about the degradation of the cytoplasmic contents within membrane bound vesicles called lysosomes.
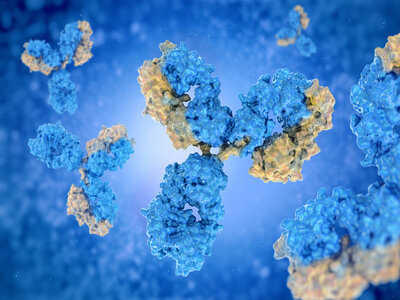
Anyone who is remotely interested in biology, or has perhaps scrolled through fitness websites to get in shape, has come across the word "protein". There is, however, much more to proteins than simply being a key player in maintaining active lifestyles. Proteins are ubiquitous in the cells of the body and are the driving force for key cellular processes. In order for proteins to carry out their duties, they need to be well-armed to execute their functions. This process of making the protein competent is achieved through specific post translational modifications (PTMs). The star of the PTMs is a cellular process called phosphorylation. The conventional methods adopted for quantifying phosphorylation are highly labor intensive. The development of phospho-specific antibodies has allowed for a huge sigh of relief from researchers due to their reputation of being quick, and detecting only phosphorylated forms of proteins in a complex mixture of phosphorylated and non-phosphorylated forms.