Remember once upon a time when I said my first actual laboratory research project involved myelin basic protein? Other than knowing that the mother of one of my high school friends had been diagnosed with it, this was the first real exposure I had with multiple sclerosis. I eventually learned more about the immune system and autoimmunity, and the thought of your own body attacking your literal nerve cells was scary and made me feel for the people who have to live with and manage this disease every day. March happens to be Multiple Sclerosis Awareness Month, which as the name suggests works to make sure the public knows about multiple sclerosis, develops empathy and understanding for afflicted individuals, and encourages participation in events and activities to spread awareness. In this blog, let's explore the disease, current treatment strategies and ongoing research, and ways that you can help both in and out of the lab.
Remember once upon a time when I said my first actual laboratory research project involved myelin basic protein? Other than knowing that the mother of one of my high school friends had been diagnosed with it, this was the first real exposure I had with multiple sclerosis. I eventually learned more about the immune system and autoimmunity, and the thought of your own body attacking your literal nerve cells was scary and made me feel for the people who have to live with and manage this disease every day. March happens to be Multiple Sclerosis Awareness Month, which as the name suggests works to make sure the public knows about multiple sclerosis, develops empathy and understanding for afflicted individuals, and encourages participation in events and activities to spread awareness. In this blog, let's explore the disease, current treatment strategies and ongoing research, and ways that you can help both in and out of the lab.
What is Multiple Sclerosis?
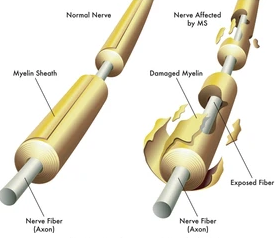 Multiple sclerosis (MS) is a debilitating autoimmune disease in which the body's immune system attacks the myelin surrounding nerve fibers. Myelin not only serves as a protective sheath, but also accelerates nerve signals and allows proper communication throughout the brain and the rest of the nervous system. Demyelination, or the destruction of this protective myelin sheath, leads to disruptions in nervous communication. Symptoms may vary dependent on the extent of demyelination, but can include changes in sensation, the loss of fine motor control, vision issues, or the ability to walk. Most MS patients have what is termed a "relapsing-remitting" MS (RRMS) in which symptoms can arise suddenly over a variable period of time, followed by recovery and prolonged periods of remission, making the disease course very unpredictable.
Multiple sclerosis (MS) is a debilitating autoimmune disease in which the body's immune system attacks the myelin surrounding nerve fibers. Myelin not only serves as a protective sheath, but also accelerates nerve signals and allows proper communication throughout the brain and the rest of the nervous system. Demyelination, or the destruction of this protective myelin sheath, leads to disruptions in nervous communication. Symptoms may vary dependent on the extent of demyelination, but can include changes in sensation, the loss of fine motor control, vision issues, or the ability to walk. Most MS patients have what is termed a "relapsing-remitting" MS (RRMS) in which symptoms can arise suddenly over a variable period of time, followed by recovery and prolonged periods of remission, making the disease course very unpredictable.
According to the National Multiple Sclerosis Society, about a million people in the United States have MS as of 2019. The disease, which can affect a variety of people, is not directly heritable or contagious, and the exact cause of the disease is still unknown, but scientists have outlined many factors that could predispose certain populations to MS. Factors such as gender, age, even where the person lives can increase the odds of someone developing MS. For example, as of 2017, three times as many women have MS compared to men, suggesting that there may be a hormonal contribution to disease progression.
At this time, there is no cure for MS, but medical science has developed many therapies to help patients recover from bouts of MS and to manage symptoms. Find out more from the Mayo Clinic by watching this video:
Potential Biomarkers of MS
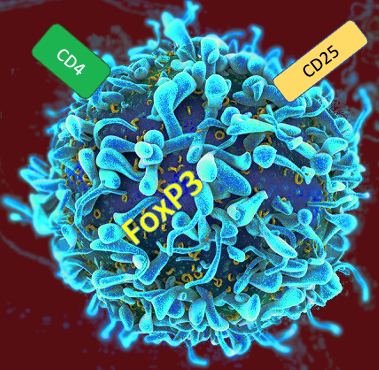
I mentioned myelin basic protein (MBP) above, as it is one of the most abundant proteins found in myelin, and happens to be the most widely studied myelin protein associated with MS. 1, 2 In my structural biology project, we tried to get MBP, an intrinsically disordered protein structure, to crystallize in a two-dimensional lattice using a negatively charged lipid to aggregate the highly positively charged protein. Later on I discovered that MBP could form short ordered alpha-helical structures, but the most studied role of MBP is as a potential autoantigen in MS. The prevailing theory is that MBP may be exposed to the immune system when myelin loosening occurs, given that MBP can be found in the cerebrospinal fluid (CSF) along with many other markers. 1-3 There is plenty of evidence of both T and B cell infiltration and activation into the central nervous system of MS patients, particularly in the presence of autoantibodies in patient samples. 3-5
Common markers being studied in an effort to generate better diagnostic and therapeutic tools for multiple sclerosis include the apolipoproteins, such as Apolipoprotein E, retinol binding protein 4 (RBP4), and many proteins found in CSF samples. 3 Besides MBP, other myelin-associated proteins and proteins involved in neural function and maintenance include heat shock proteins such as crystallin alpha B, membrane proteins that include the aquaporins, and membrane proteins such as MOG. 5 Assessing the relative levels of these markers compared to non-MS CSF can help gauge severity and guide treatment options for the individual MS patient. The Mayo Clinic has rolled out a rapid antibody test to diagnose MS via CSF analysis as of last year.
Treatment Options for MS
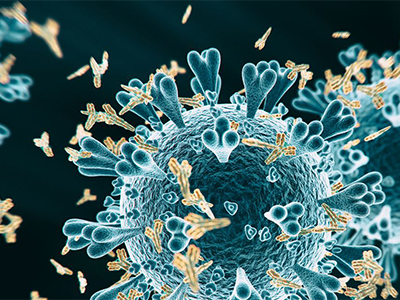 I am always making fun of the drug commercials where they sort of say what the drug does for about five seconds before they spend the next ten minutes telling you all the ways it can kill you. With no cure as of yet, the best current method to combat MS and help patients live as normal of a life as they can is to manage the symptoms and reduce the risk of relapse. There are various treatment options available for people suffering from autoimmune diseases, and some of these strategies have been adapted to treat MS. One of the drug commercials that I am intimately familiar with because it plays about 80 times in a typical sporting event is Ocrevus, an anti-CD20 therapy produced by Genentech/Roche. CD20 is an identifying surface marker on B lymphocytes that regulate their differentiation and function, and common antibody-mediated treatments, including Ocrevus, target CD20 in order to reduce the number of circulating B cells and suppress the autoimmune response in MS patients. 6, 7 For Ocrevus in particular, the data shows that the drug reduced relapses and slowed disease progression in RRMS patients, which also reduced the prevalence of physical disability in patients who took the drug.
I am always making fun of the drug commercials where they sort of say what the drug does for about five seconds before they spend the next ten minutes telling you all the ways it can kill you. With no cure as of yet, the best current method to combat MS and help patients live as normal of a life as they can is to manage the symptoms and reduce the risk of relapse. There are various treatment options available for people suffering from autoimmune diseases, and some of these strategies have been adapted to treat MS. One of the drug commercials that I am intimately familiar with because it plays about 80 times in a typical sporting event is Ocrevus, an anti-CD20 therapy produced by Genentech/Roche. CD20 is an identifying surface marker on B lymphocytes that regulate their differentiation and function, and common antibody-mediated treatments, including Ocrevus, target CD20 in order to reduce the number of circulating B cells and suppress the autoimmune response in MS patients. 6, 7 For Ocrevus in particular, the data shows that the drug reduced relapses and slowed disease progression in RRMS patients, which also reduced the prevalence of physical disability in patients who took the drug.
Other than humanized anti-CD20 antibody treatments, strategies to slow the progression of the disease and manage symptoms include corticosteroids and interferon beta to reduce nerve inflammation and potential disease-mediated inflammation, and fumarate medications to reduce relapse risk. More recent treatments being explored include BTK inhibitors, which were first developed as cancer treatments but have been adapted by pharmaceutical companies to also fight MS. Despite not having a cure yet, the research has come a long way to making MS patient lives more fulfilling and comfortable.
UPDATE: There is an excellent review article about MS and therapeutic targeting in Cell in the March 30, 2023 issue that offers a look at emerging paths in studying and treating the disease. 8
How You Can Raise MS Awareness
There are many organizations dedicated to helping people living with MS and raising funds and awareness for the disease. These include the Multiple Sclerosis Foundation and the National Multiple Sclerosis Society, with events like gatherings and challenge walks or bicycle rides going on throughout the year and particularly during Multiple Sclerosis Awareness Month. You can donate either your time or any disposable income you see fit towards research and aid for MS patients in their everyday lives, including support equipment and medical treatments.
If you're interested in ABclonal antibodies to the markers discussed in this blog for your own research, feel free to click through on the target names I sprinkled throughout the blog, and also to contact us at service@abclonal.com for more information. Together, we can work towards a better future for MS patients.
References
- Rozenblum GT, Kaufman T & Vitullo AD (2014) "Myelin Basic Protein and a Multiple Sclerosis-related MBP-peptide Bind to Oligonucleotides." Mol Ther Nucleic Acids 3(9):e192 (Epub).
- Martinsen V & Kursula P (2022) "Multiple sclerosis and myelin basic protein: insights into protein disorder and disease." Amino Acids 54:99-109.
- Salazar et al. (2022) "Posttranslational modifications of proteins are key features in the identification of CSF biomarkers of multiple sclerosis." Journal of Neuroinflammation 19:44 (Epub).
- Weber MS, Hemmer B & Cepok S (2011) "The role of antibodies in multiple sclerosis." Biochimica et Biophysica Acta - Molecular Basis of Disease 1812(2):239-245.
- Kuerten et al. (2020) "Autoantibodies against central nervous system antigens in a subset of B cell-dominant multiple sclerosis patients." PNAS 117(35):21512-21518.
- Voge NV & Alvarez E (2019) "Monoclonal Antibodies in Multiple Sclerosis: Present and Future." Biomedicines 7(1):20 (Epub).
- Roach CA & Cross AH (2021) "Anti-CD20 B Cell Treatment for Relapsing Multiple Sclerosis." Front Neurol 11:595547 (Epub).
- Charabati et al. (2023) "Multiple sclerosis: Neuroimmune crosstalk and therapeutic targeting." Cell 186(7):1309-1327.